THIS ARTICLE IS MORE THAN FIVE YEARS OLD
This article is more than five years old. Autism research — and science in general — is constantly evolving, so older articles may contain information or theories that have been reevaluated since their original publication date.
Roughly 7 percent of children with autism eventually lose their diagnosis, swapping social problems and language difficulties for more typical skills and behaviors. But it is unclear whether this transition is associated with a return to typical brain function or reflects a compensatory process.
New findings support the second possibility. They suggest that children who achieve a so-called ‘optimal outcome’ have unusually active language regions in the brain relative to children with mild autism or those without the condition1.
“The complete normalization of language skills that we observe in children with optimal outcomes from autism seems to reflect a rather atypical organization at the level of the brain,” says study researcher Inge-Marie Eigsti, associate professor of psychology at the University of Connecticut.
Children who achieve an optimal outcome may receive earlier and more intense autism treatments than children who keep their autism diagnosis, according to a 2014 report by Eigsti’s group in the Journal of Developmental and Behavioral Pediatrics2. The new study, which appeared in December in NeuroImage: Clinical, suggests these early interventions spark compensatory brain changes rather than promoting neurotypical brain development.
“This finding gives us insight into how brains respond to intervention in autism, and has the potential to inform intervention strategies and monitoring of response to intervention in autism in the future,” says Lisa Shulman, director of the RELATE program for children with autism at Albert Einstein College of Medicine in New York, who was not involved in the research.
Paper trail:
Eigsti and her team studied 59 children and young adults, 8 to 21 years old, including 20 typically developing participants and 39 who were diagnosed with mild autism before age 5. Of the individuals with mild autism, 16 later lost their diagnosis.
To confirm these diagnoses, the researchers reviewed each child’s medical records and used a clinical checklist for autism called the Autism Diagnostic Observation Schedule (ADOS). They also used the Autism Diagnostic Interview-Revised (ADI-R), which relies on parent or caregiver reports to document a child’s history of autism behaviors, and the Wechsler Abbreviated Scale of Intelligence, which measures cognitive ability.
The researchers then monitored brain activity with functional magnetic resonance imaging as participants responded to short true-or-false questions that tested their ability to comprehend written language.
Eigsti says she expected the children who had shed their autism diagnosis to show brain activity that mirrors the brain activity seen in the control group and not the autism group. Instead, those children showed a unique signature of brain activity that reflects a tendency to compensate for difficulty with language.
Activity burst:
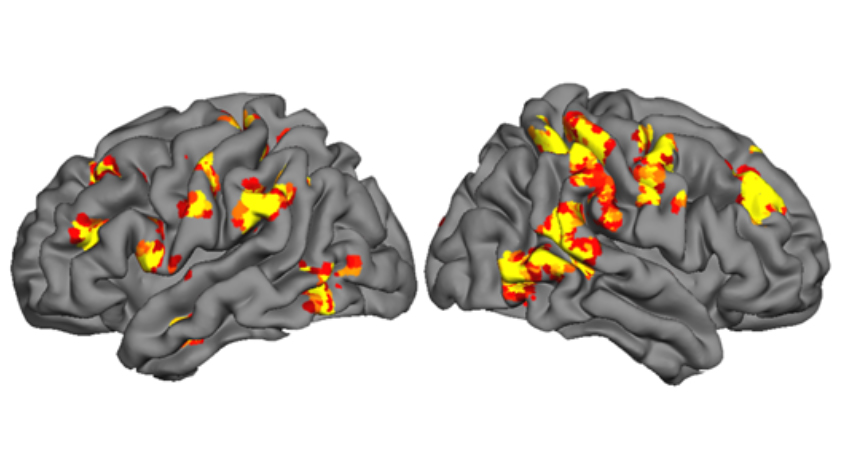
In all of the participants, the tasks activated left brain language regions such as Broca’s area, which controls speech, as well as regions governing cognitive control, motor skills and motivation. Children with a history of autism also recruited regions in the right hemisphere to help with the language tasks. But those who cast off the diagnosis showed the highest levels of activation in all of the relevant language, cognitive and motor regions.
The results held up even when the researchers controlled for age, gender and intelligence level.
This new information could help researchers understand how early interventions affect the developing brain. “One common characteristic of our kids with optimal outcomes is that they’ve begun receiving behavioral interventions really quite early, even as early as 18 to 24 months,” Eigsti says. “We think that’s a really important piece of the story.”
Eigsti and her team plan to explore how this unique brain activity signature emerges over time in children with autism as they catch up with their typically developing peers.
By joining the discussion, you agree to our privacy policy.