Genes
Mutation in top autism-linked gene may alter eye reflex
The discovery could help clinicians diagnose children who carry mutations in the gene, called SCN2A, and gauge their responses to potential therapies.
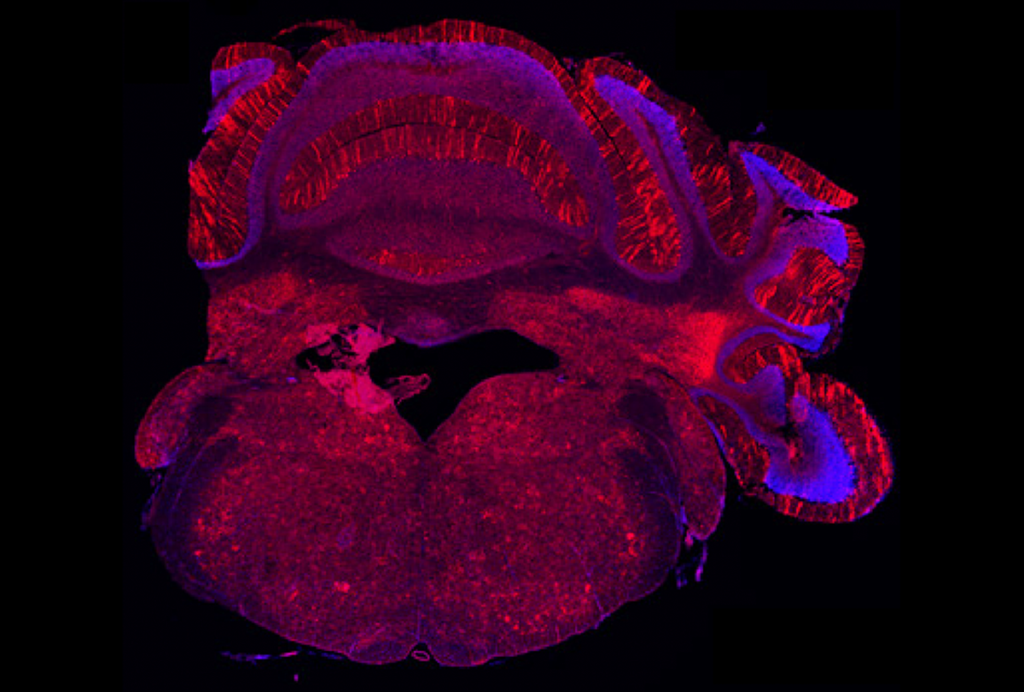
Mutation in top autism-linked gene may alter eye reflex
Some social issues in DYRK1A model mice stem from faulty inhibitory circuits
Alterations in inhibitory circuits and difficulties in social recognition characterize mice missing one copy of DYRK1A, a gene linked to autism.
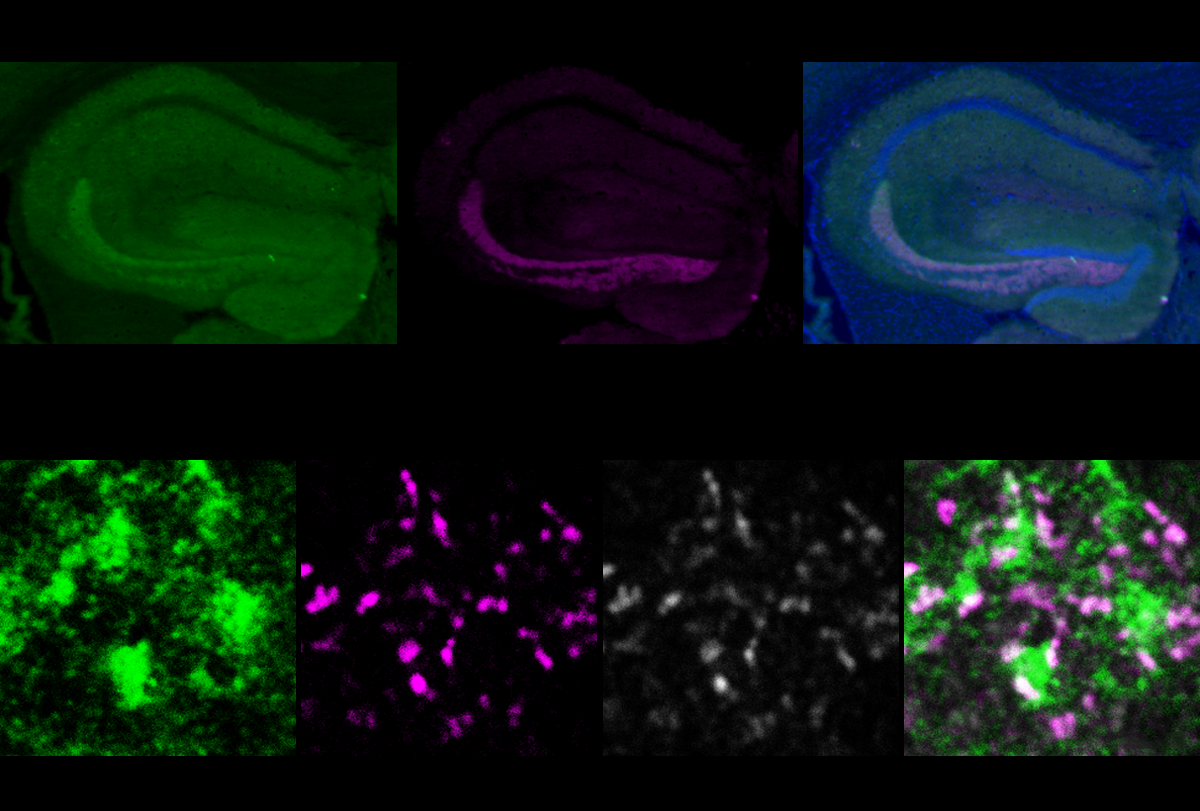
Some social issues in DYRK1A model mice stem from faulty inhibitory circuits
UBE3A’s link to synaptic pruning bolstered by fly study
Increasing or reducing the levels of the UBE3A gene, which is associated with autism and autism-related syndromes, results in altered patterns of synaptic pruning — a process that snips away brain cell connections.
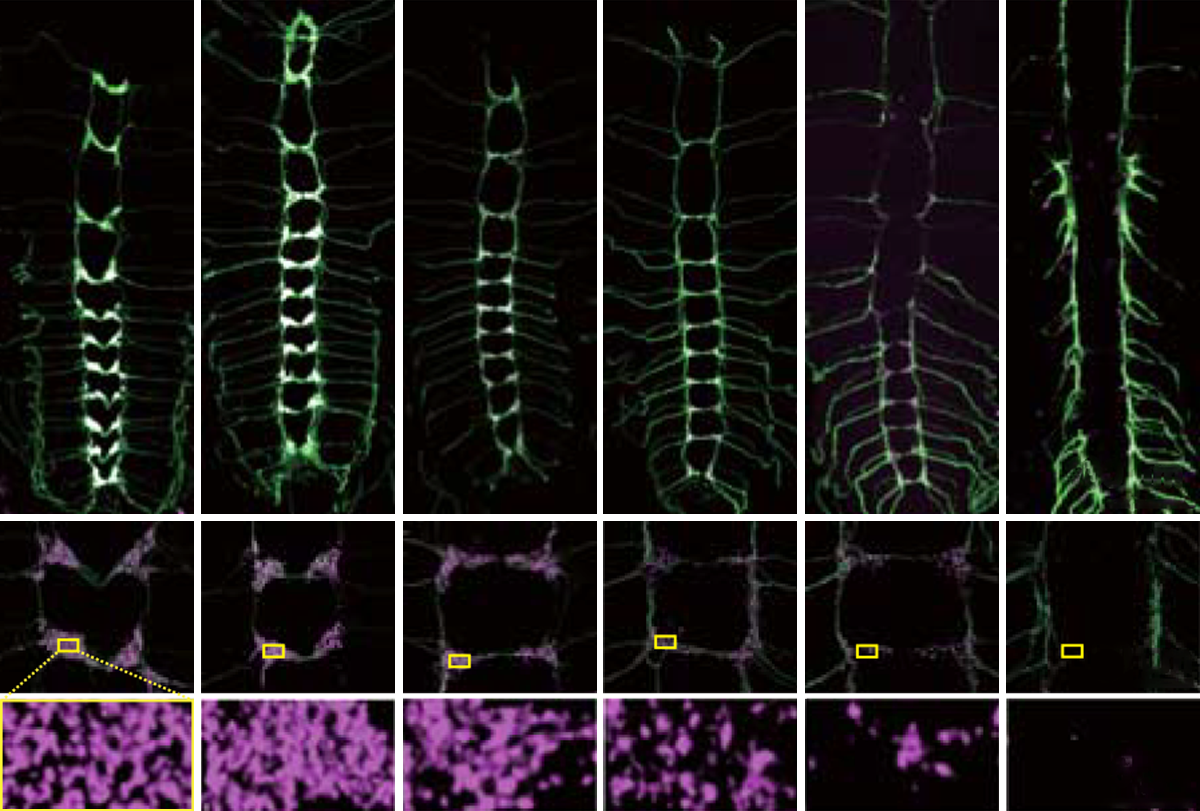
UBE3A’s link to synaptic pruning bolstered by fly study
Head size parts autism into two major subtypes
An imbalance in the number of excitatory neurons in early brain development may account for the difference.
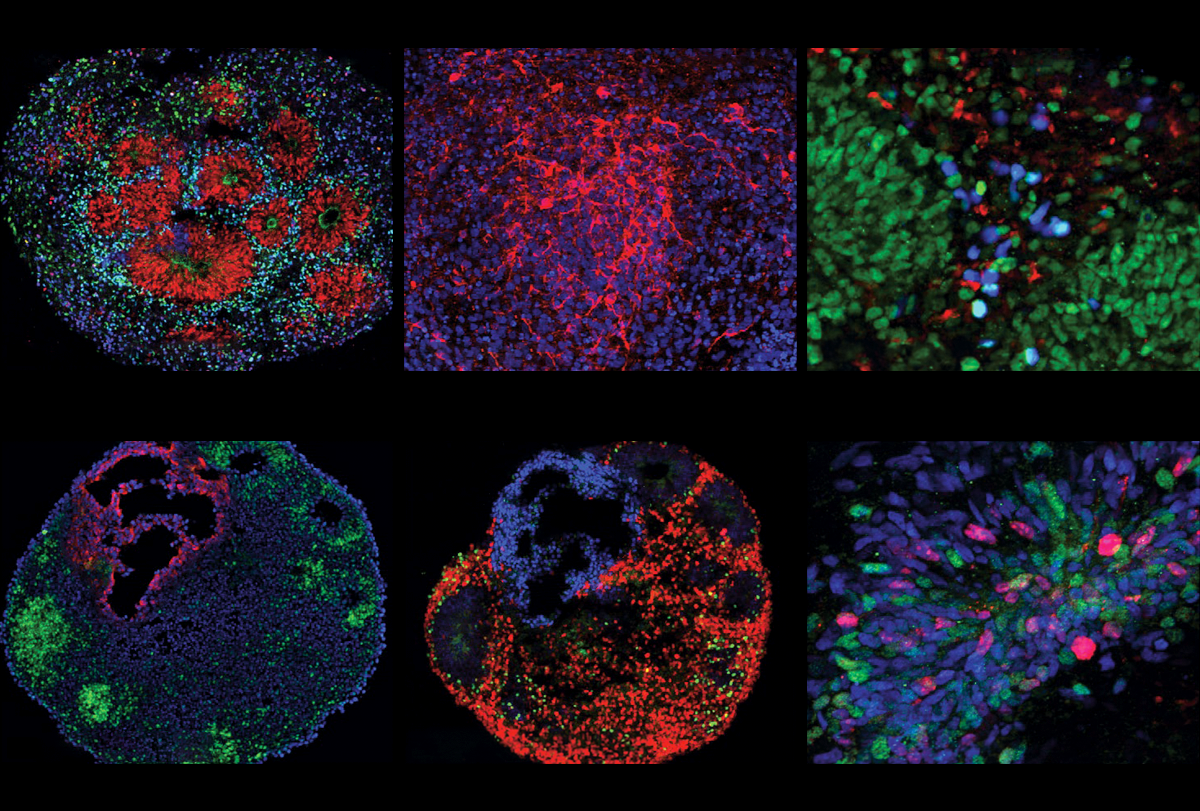
Head size parts autism into two major subtypes
Skewed signaling in striatum may spawn repetitive behaviors
Synaptic changes in the brain region could drive a core trait of fragile X syndrome, a new mouse study suggests.
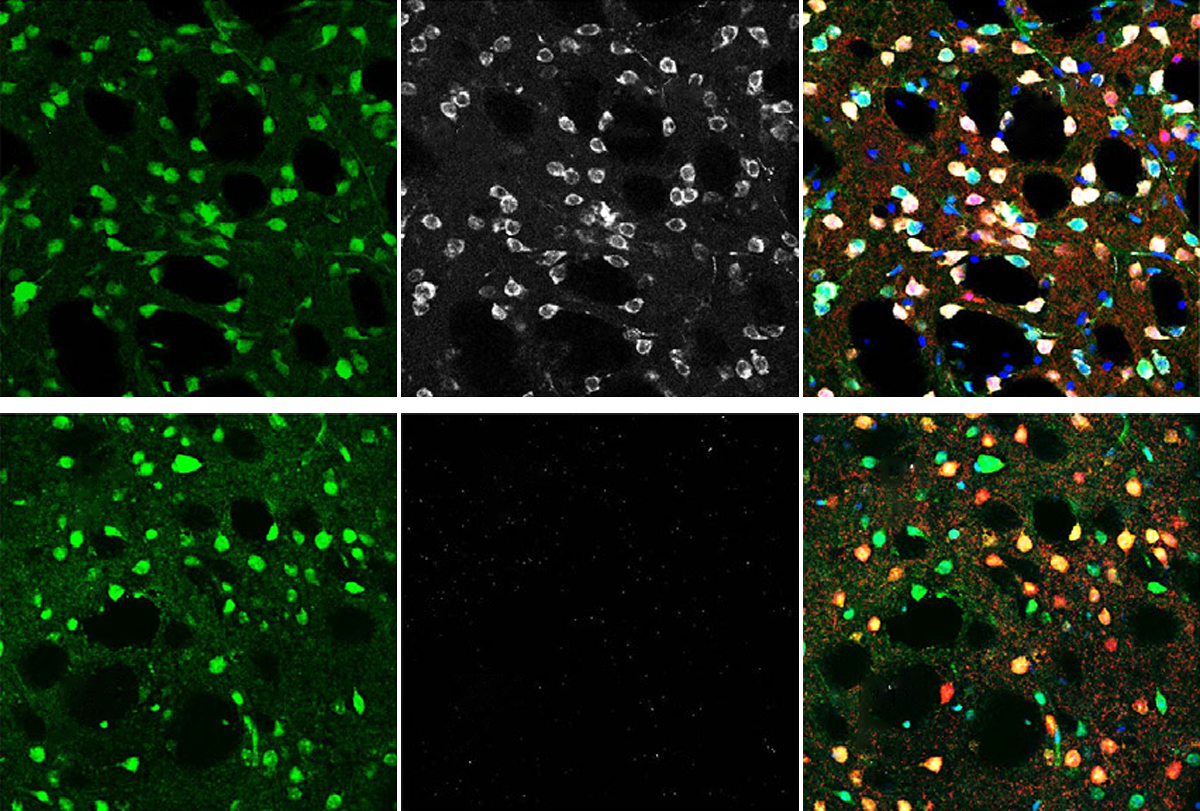
Skewed signaling in striatum may spawn repetitive behaviors
Father’s genes may drive sociability in male monkeys
The findings in rhesus macaque monkeys may provide clues to sex differences in the heredity of social behavior in people.

Father’s genes may drive sociability in male monkeys
New test taps nose pokes as a proxy for social motivation in mice
Over one hour, a particularly motivated mouse poked its nose 350 times into a hole in the test chamber in the hopes of meeting a playmate.
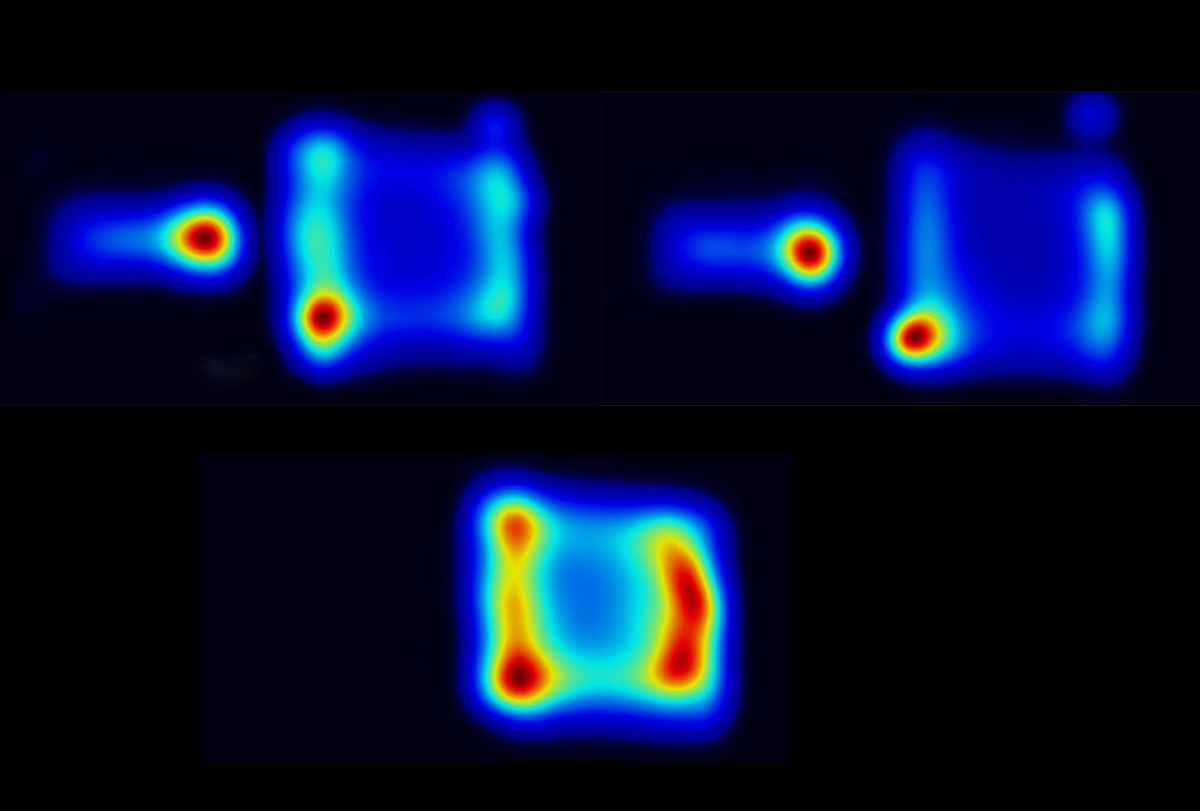
New test taps nose pokes as a proxy for social motivation in mice
Abundant motor proteins disrupt cries in FOXP2 mice
Knocking down the gene that codes for the proteins normalizes the vocalizations.
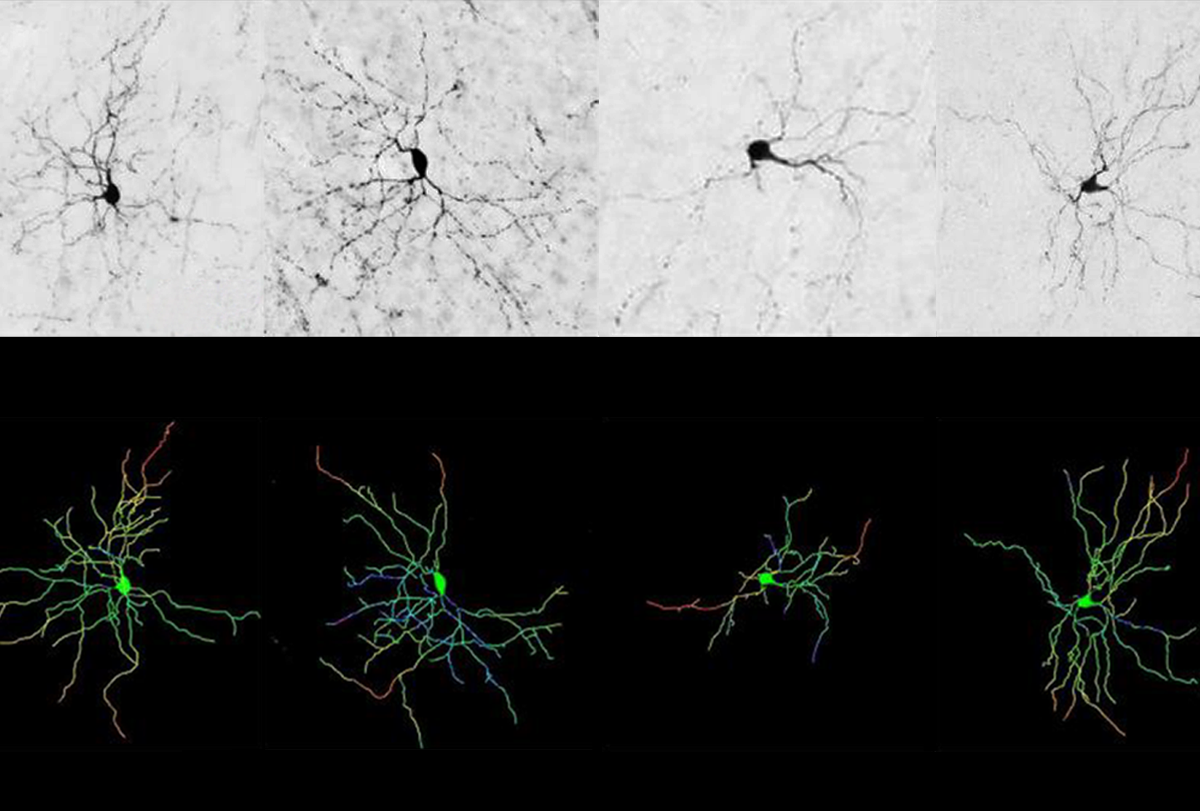
Abundant motor proteins disrupt cries in FOXP2 mice
‘Gain-of-function’ mutation spawns autism traits
The mutation increases the activity of an autism-linked protein and leads to social difficulties and other behavioral differences in mice.
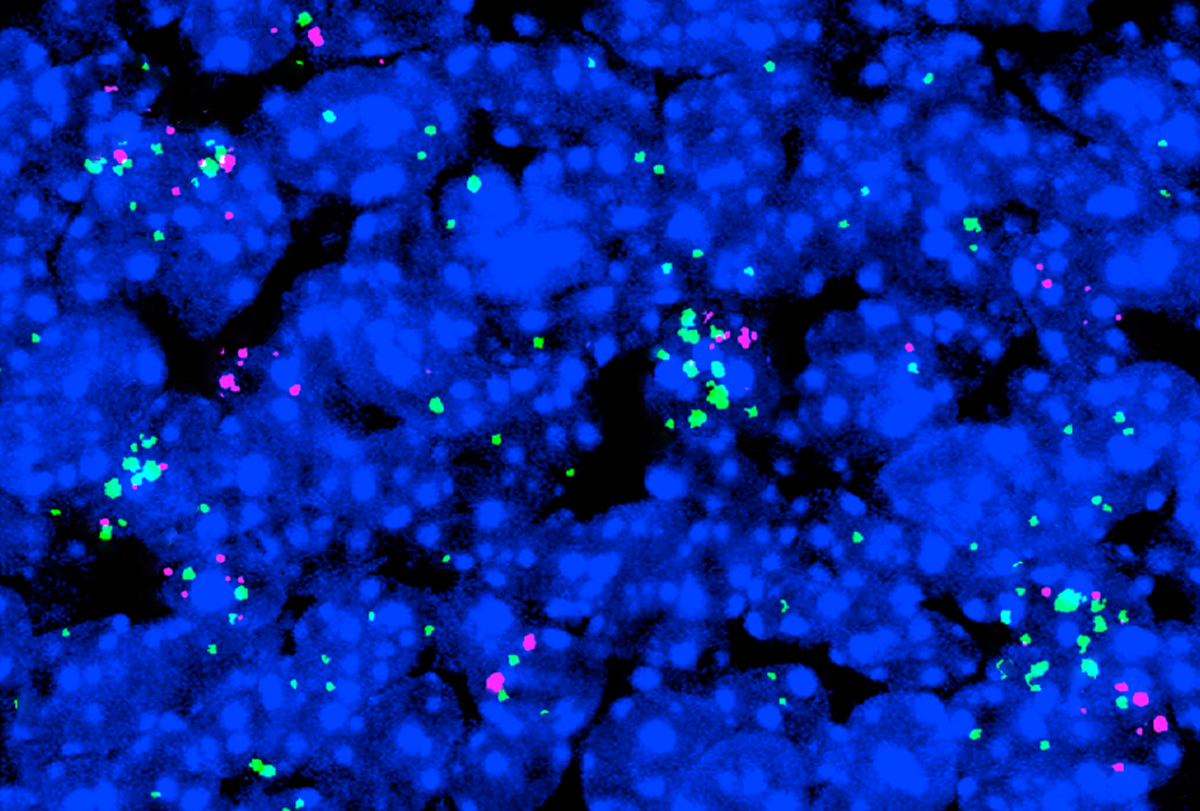
‘Gain-of-function’ mutation spawns autism traits
‘VIP’ interneurons may drive autism traits in Dravet syndrome
The inhibitory cells misfire and contribute to social difficulties in mice that model the syndrome.

‘VIP’ interneurons may drive autism traits in Dravet syndrome
Explore more from The Transmitter
Crowdsourcing to curb aggression in autism: Q&A with Matthew Goodwin
To accelerate the development of real-time behavioral prediction technology, a research team is sharing data and seeking new collaborators.

Crowdsourcing to curb aggression in autism: Q&A with Matthew Goodwin
To accelerate the development of real-time behavioral prediction technology, a research team is sharing data and seeking new collaborators.
Brain connectivity and letting the data speak with Emily Finn
The Dartmouth College researcher talks about her quest to understand behavior and doing neuroscience “in the woods.”

Brain connectivity and letting the data speak with Emily Finn
The Dartmouth College researcher talks about her quest to understand behavior and doing neuroscience “in the woods.”
Carol Jennings, whose family’s genetics informed amyloid cascade hypothesis, dies at 70
Her advocacy work aided the discovery of a rare inherited form of early-onset Alzheimer’s disease and helped connect affected people with researchers.

Carol Jennings, whose family’s genetics informed amyloid cascade hypothesis, dies at 70
Her advocacy work aided the discovery of a rare inherited form of early-onset Alzheimer’s disease and helped connect affected people with researchers.