Chinese survey says…
Knowledge of autism in China is spotty, according to a large survey published last month.
Diagnosing autism is an evolving science but a crucial first step to understanding the disorder.

Knowledge of autism in China is spotty, according to a large survey published last month.

Two studies published in the past month highlight the challenges in balancing the accuracy of autism diagnosis with cost-effectiveness and speed.

Over the past 30 years, autism research pioneer Fred Volkmar says he has learned that researchers should be humble when assigning meaning to autism behavior, and seek to translate their findings into useful applications.

Adults with autism are more likely than controls to have certain chronic health conditions, such as high cholesterol, but are less likely to treat these with prescription drugs.

Autism prevalence is five times higher in young adults born weighing 2,000 grams or less compared with controls, according to a study published 17 October in Pediatrics.

A five-minute online questionnaire can diagnose autism with as much accuracy as the so-called gold standard diagnostic tests, according to unpublished findings presented Tuesday at the Autism Consortium 2011 symposium in Boston.

A large epidemiological study in Utah that relies on tax information and health records shows that income level does not affect the odds of having a child with autism or intellectual disability.

An autism-linked protein helps wire neurons together, according to two studies published in late September.
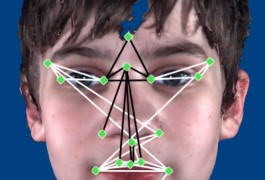
Boys with autism have a distinct facial structure that differs from that of typically developing controls, according to a study published 14 October in Molecular Autism.

Individuals with Asperger syndrome perform at the same level as controls do on tests of visual ability, according to a study published 30 August in Biological Psychiatry. This result adds to growing evidence against the claim, made in an infamous 2009 study, that individuals with autism have superior vision.