Male mice pass stress signatures down to their pups
The pups of male mice exposed to stress show a muted response to stressful situations of their own, suggesting that environmental effects can last generations.
The pups of male mice exposed to stress show a muted response to stressful situations of their own, suggesting that environmental effects can last generations.

Older women and men are at high risk of having a child with autism — and so are teenage girls and parents whose age differs by at least a decade, according to a multinational study of more than 5 million children.

When covering research on prenatal risk factors, are journalists too quick to blame the mother?

Guinea pigs have advantages over other rodent species commonly used to model disorders such as autism, according to preliminary research published Tuesday at the Society for Neuroscience annual meeting in San Diego.

Women who report being abused as children are more likely to have a child with autism, according to a new report from the Nurses’ Health Study, published 20 March in the Journal of the American Medical Association.

Maternal health seems to have little impact on autism risk, according to a study published 7 January in PLoS One. The more serious risk is for intellectual disability, which can often occur along with autism.
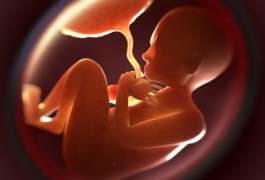
As the central organ regulating maternal-fetal interactions, the placenta is perfectly positioned to mediate environmental and genetic risk factors during prenatal development. It may also relay risk factors for autism to the fetus, says Paul Patterson.

Experiencing a stressful event during pregnancy does not increase the risk of having a child with autism, according to an epidemiological study published 13 June in PLoS One.

An untreated fever during pregnancy more than doubles the risk that the child will develop autism, according to a study published 5 May in the Journal of Autism and Developmental Disorders.

By studying pregnant women who already have a child with autism, researchers hope to understand how epigenetic changes — those that affect gene expression but don’t directly alter DNA — during pregnancy influences risk of the disorder.