Flexible brain
Transcranial magnetic stimulation may provide a noninvasive approach to studying how connections in the human brain change in response to new information, and how that process is altered in autism, says Lindsay Oberman.
 Transcranial magnetic stimulation (TMS), a noninvasive method for stimulating the brain, is an increasingly common tool in neuroscience research. Given its unique ability to directly affect the functioning of a given part of the brain, it has been used to study such things as how blind people read Braille, and the role of the frontal cortex in morality and working memory, as well as in the treatment of many neurological conditions including depression, stroke rehabilitation, Alzheimer’s and Parkinson’s diseases, schizophrenia and epilepsy.
Transcranial magnetic stimulation (TMS), a noninvasive method for stimulating the brain, is an increasingly common tool in neuroscience research. Given its unique ability to directly affect the functioning of a given part of the brain, it has been used to study such things as how blind people read Braille, and the role of the frontal cortex in morality and working memory, as well as in the treatment of many neurological conditions including depression, stroke rehabilitation, Alzheimer’s and Parkinson’s diseases, schizophrenia and epilepsy.
We are using TMS to study how the synapses, or connections between neurons, change in response to new information, a process called synaptic plasticity.
Synaptic plasticity is of particular interest in autism. Data from animal models and genetic studies suggest that defects in synaptic plasticity may be core impairments in people with the disorder.
In rodents, we can study problems with synaptic plasticity directly, using invasive molecular and physiologic neuroscience techniques. In the human brain, TMS has emerged as a noninvasive method to study these same processes (albeit on a larger scale) in ways previously not accessible.
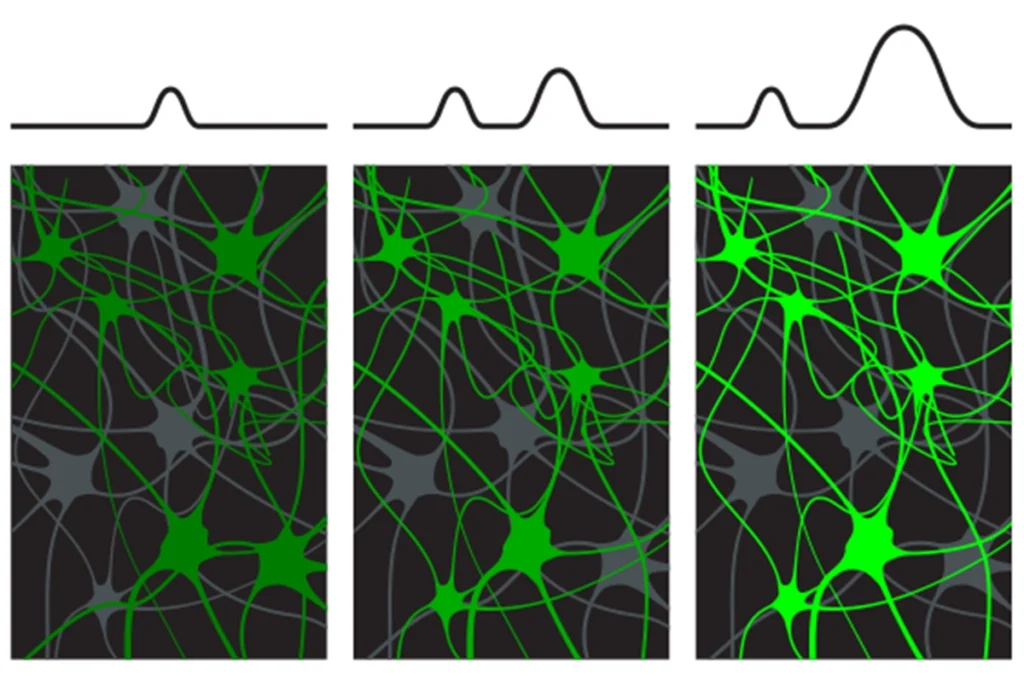
Neurons undergo two types of synaptic plasticity: long-term potentiation (LTP), which increases the strength of the connection between cells, and long-term depression (LTD), which decreases the strength. Though we can’t directly measure LTP and LTD in the living human brain, studies have shown that a specific pattern of repeated stimulation with TMS can induce LTP- and LTD-like responses in the cortex.
According to our published work, high-functioning adults with autism show an abnormal response to this pattern of stimulation. The effects are more pronounced and longer lasting than those in controls matched by age, gender and intelligence quotient.
Specifically, intermittent stimulation makes the cortex more excitable both in people with autism and in controls, but the autism group shows a stronger response than controls do. Conversely, continuous stimulation dampens excitability in both groups but suppresses it more in people with autism than in controls.
Our preliminary data suggest that this response is more pronounced in high-functioning individuals with autism than in those who are more impaired. However, we have so far only studied a few low-functioning individuals with autism.
The findings may help explain some of the neural and behavioral problems in people with autism. If infants and children with the disorder show abnormal synaptic plasticity, their neural circuits are likely to develop incorrectly. That may lead to a breakdown in communication across the cortex, and in turn trigger behavioral symptoms.
The patterns we see may also reflect a noisier brain — meaning that important neural signals are difficult to pick out from background noise. That may slow down complex processing, such as that needed for social interaction and communication. It may also explain the higher incidence of epilepsy in this population.
The findings beg for a more thorough examination of plasticity mechanisms in the wider autism spectrum population. We plan to use TMS to analyze plasticity in adults and children with autism over time — as with other symptoms, these deficits may change with age. We are also investigating how changes in plasticity are linked to behavioral symptoms.
If further research confirms this abnormal response in people with autism, and shows that these changes are linked to behavior, the next step would be to examine whether modifying brain activity to a more typical pattern, either with drugs or perhaps even with TMS, can alter behavior.
Lindsay Oberman is an instructor in neurology at Beth Israel Deaconess Medical Center in Boston.
Explore more from The Transmitter
Cocaine, morphine commandeer neurons normally activated by food, water in mice
X chromosome inactivation; motor difficulties in 16p11.2 duplication and deletion; oligodendroglia
