THIS ARTICLE IS MORE THAN FIVE YEARS OLD
This article is more than five years old. Autism research — and science in general — is constantly evolving, so older articles may contain information or theories that have been reevaluated since their original publication date.
A method that maps signaling molecules in the brain may help researchers home in on epileptic lesions — structurally abnormal brain areas where seizures originate. The technique may identify individuals with drug-resistant epilepsy who could benefit from surgery to remove the problematic lesions1.
Roughly 25 percent of people with autism also have epilepsy. In a study published in June that looked at people who have both disorders, one-quarter of the males and nearly half of the females have seizures that do not respond to medication.
Surgery to remove small pieces of the problematic brain tissue can ease drug-resistant epilepsy. The surgery is most effective when doctors use magnetic resonance imaging (MRI) to pinpoint lesions. But in some people, the MRI misses lesions that pathologists later discover2. Opening up the skull to record electrical activity within brain tissue can provide additional clues about a lesion’s location, but the procedure carries risks.
The new method, described 14 October in Science Translational Medicine, uses a modified type of MRI — called glutamate chemical exchange saturation transfer (GluCEST) — to hunt for lesions. GluCEST noninvasively tracks the distribution of the neurotransmitter glutamate, which excites neurons3. Abnormal glutamate buildup is associated with epilepsy and can lead to seizures. The researchers hypothesized that GluCEST might detect elevated glutamate at seizure hotspots even in cases where structural abnormalities had not shown up in a conventional MRI.
The researchers used GluCEST to look at the brains of 4 people with uncontrolled epilepsy and 11 controls. All of the individuals with epilepsy had seizures that appeared to originate in the temporal lobe (a quadrant of the brain that sits under the ears), but standard MRI had not revealed the specific lesions.
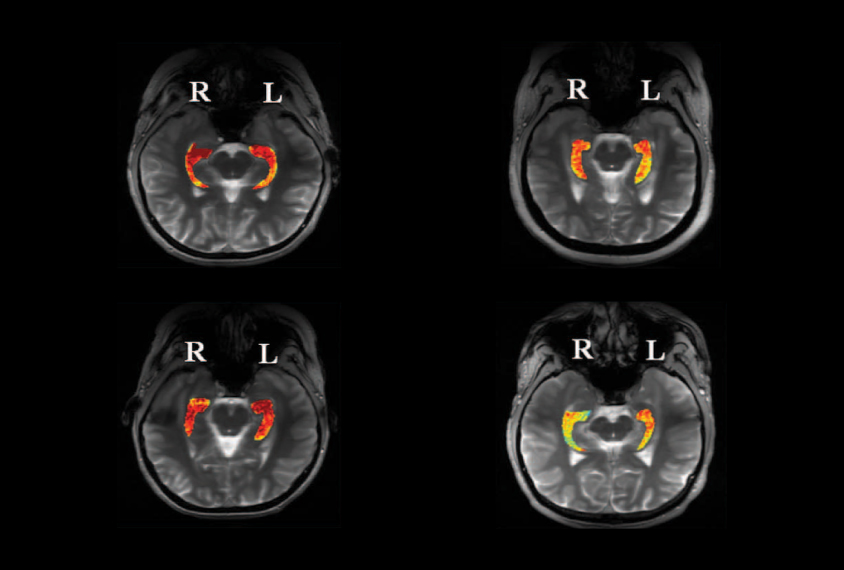
Using GluCEST, the researchers uncovered areas of high glutamate concentration within the hippocampus, a brain region within the temporal lobe that modulates memory. The method revealed that two of the individuals had epileptic lesions in the left hippocampus, and two had them in the right.
In one of the four individuals, doctors recorded electrical seizure activity in her brain prior to surgery. They deduced that the seizures originated in the right side of the brain — consistent with the GluCEST findings. The individual went on to have part of her right hippocampus removed, and pathologists confirmed that the excised tissue was likely the site of an epileptic lesion.
The researchers acknowledge that the study is small and only included individuals with seizures originating in the temporal lobe. Future work may reveal whether GluCEST can illuminate seizure hotspots in other parts of the brain.
By joining the discussion, you agree to our privacy policy.