THIS ARTICLE IS MORE THAN FIVE YEARS OLD
This article is more than five years old. Autism research — and science in general — is constantly evolving, so older articles may contain information or theories that have been reevaluated since their original publication date.
A sweeping study of military health records reveals that children with autism are at risk for a host of obesity-related health issues, such as high blood pressure and diabetes. These issues are especially common among children who take drugs to ease autism features1.
The findings highlight the complexity of treating anxiety and repetitive behaviors in children with autism without creating or exacerbating chronic health problems. These children often have trouble controlling their weight even when not taking medications, because many are picky eaters or get little exercise.
But “sometimes children with autism do need to be medicated,” says lead researcher Cade Nylund, assistant professor of pediatrics at the Uniformed Services University of the Health Sciences in Bethesda, Maryland. “Parents need to understand the risks; providers need to explain the risks.”
The study, published in August in the Journal of Pediatrics, is the largest yet to explore autism’s ties to obesity. Nylund’s team examined military health records from 292,572 children aged 2 to 18, including 48,762 children with autism. The researchers compared rates of obesity, type 2 diabetes, and cardiovascular and liver disease in children with and without autism (see graphic below). They also looked at the impact of medication use on obesity rates in children with autism.
The analysis revealed that about 8.2 percent of children with autism are obese compared with 4.7 percent of typical children.
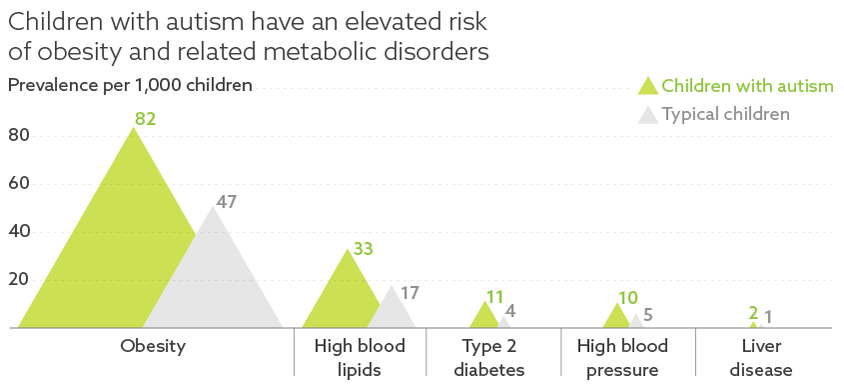
Graphic by Lucy Reading-Ikkanda
These rates are much lower than those reported in another study of 43,777 children, published 5 October in Childhood Obesity. That study set the prevalence of obesity among children with autism at 23 percent compared with 14 percent of controls2. But it looked at children 10 to 17 years old, and raises the possibility that obesity prevalence shifts with age.
Weight list:
The military records study shows that children with autism who take drugs for anxiety, depression or inattention are at a higher risk of obesity than are unmedicated children with autism. Specifically, the researchers found that mood stabilizers raise the odds of obesity by 40 percent. Antipsychotic drugs, such as risperidone, are linked to an almost 20 percent increase in obesity prevalence, but drugs used to treat hyperactivity and inattention have minimal effects on body weight.
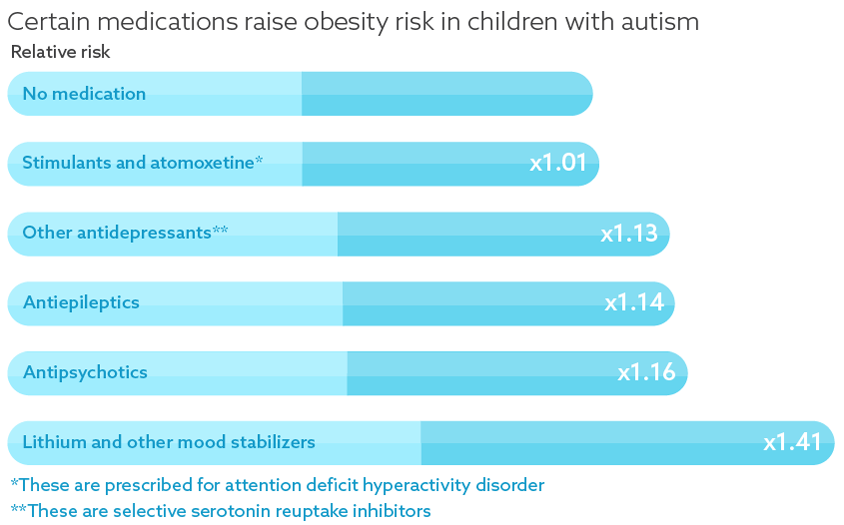
Graphic by Lucy Reading-Ikkanda
Overall, children with autism are more likely than those without the condition to develop obesity-related health issues. Diabetes is about three times as common in children with autism as in the general population. And children with autism are twice as likely as controls to have high blood pressure or elevated cholesterol.
Pediatricians often counsel children with weight-related health problems to exercise and eat a healthy diet. But because these lifestyle remedies can be challenging for children with autism, some clinicians prescribe additional medications to manage obesity and its consequences.
The diabetes drug metformin, for instance, can reverse weight gain in children with autism who take antipsychotic medications. Medications such as diuretics, which fight fluid retention, do not help children lose weight but address complications such as high blood pressure.
Better yet, experts say, would be to prevent obesity in the first place — by helping parents cultivate healthy habits in their children and fully understand medications’ side effects. “It’s very difficult to address these issues once a child with autism is 17 years old and overweight,” Nylund says. “The number one thing is prevention.”

By joining the discussion, you agree to our privacy policy.