THIS ARTICLE IS MORE THAN FIVE YEARS OLD
This article is more than five years old. Autism research — and science in general — is constantly evolving, so older articles may contain information or theories that have been reevaluated since their original publication date.
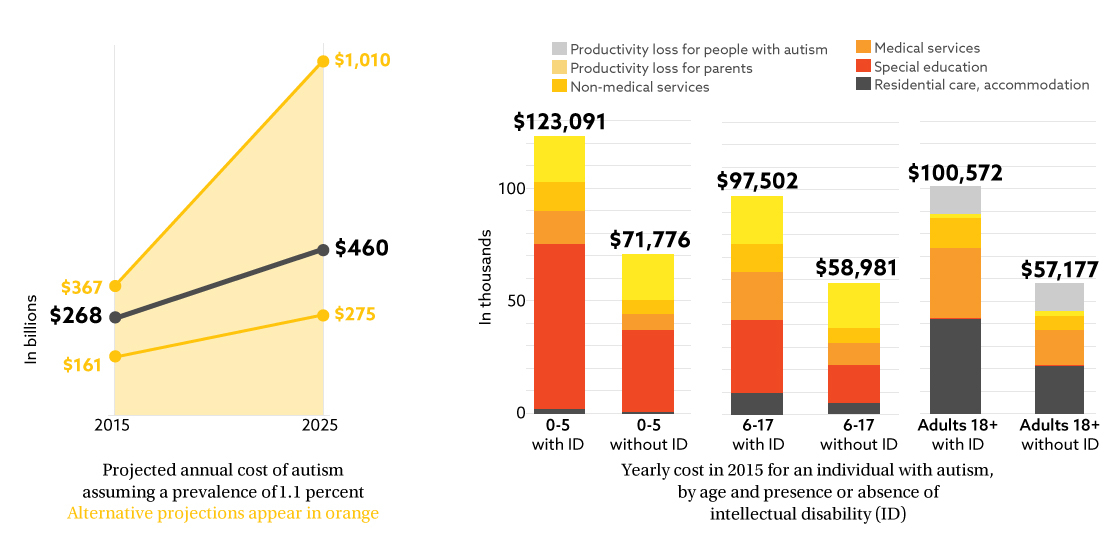
Autism will cost the U.S. $268 billion this year — roughly 1.5 percent of the country’s gross domestic product1. By 2025, the price tag could balloon to $461 billion.
These estimates, published in July in the Journal of Autism and Developmental Disorders, are the first to forecast the costs of autism a decade into the future. They assume an autism prevalence of 1.1 percent and that 40 percent of people with autism have intellectual disability, one indicator of autism severity.
“Autism is very expensive for the entire economy and, in general, for society,” says lead researcher J. Paul Leigh, professor of health economics at the University of California, Davis. “It’s more expensive than I think most people realize.”
The ‘cost’ of autism for 2015 is roughly on par with a 2012 estimate for diabetes and more than five times that of stroke or hypertension in 2010. If autism’s expense rises as predicted, it will quickly surpass that of diabetes, considered one of the country’s biggest public health problems, says Leigh.
The exact size of the bill is less important than knowing that the rising costs are unsustainable, says David Mandell, associate professor of psychiatry and pediatrics at the University of Pennsylvania. “What we need now is to ask, ‘What are we going to do about it?’”
Averting crisis:
In a 2014 study, Mandell and his colleagues found that the lifetime cost of autism for one individual is $1.4 million. That number jumps to $2.4 million for a person who also has intellectual disability2.
The new study builds off those estimates, calculating total societal costs for 2015 and 2025 using population estimates from the 2012 national census, and adjusting for inflation in medical costs and productivity.
The costs span several categories: special education, medical services, non-medical services such as after-school programs, loss of productivity (of parents and individuals with autism) and residential care.
Some of these costs are “good” — that is, designed to help affected individuals, says Martin Knapp, professor of social policy at the London School of Economics and Political Science, who was not involved in the new study. “Bad” costs, by contrast, are consequences of poor support — for example, a parent having to leave work to care for her child.
“We need to spend the money so that it’s more focused on evidence-based interventions and less focused on crisis,” Knapp says.
Because costs vary across a lifetime, the studies break them down by age: 5 years and under, 6 to 17 years, and adults. They also separate individuals with autism who have intellectual disability from those who don’t. The former often have a higher need for services.
Intellectual disability is, however, a crude way to account for the wide range in abilities across people with autism, says Maureen Durkin, professor of population health sciences and pediatrics at the University of Wisconsin-Madison.
“If we actually knew what percentage of people with autism are able to work and the impact of autism on someone’s family income, that would help narrow this a lot better,” she says. “It just shows how little we know about costs.”
Looking ahead:
For 2025, the authors applied the same 1.1 prevalence rate to a population projection for that year. But assuming a stable rate of 1.1 percent for all individuals with autism may result in a conservative estimate.
The latest report from the U.S. Centers for Disease Control and Prevention finds that 1.47 percent of 8-year-old children have autism. Extrapolating this rate to all people with autism puts costs at roughly $358 billion in 2015 and $616 billion in 2025. Assuming that autism rates will continue to climb as they have over the past few years lifts the 2025 estimate to more than $1 trillion.
But the projected costs for 2025 assume business as usual, says Mandell. “In some ways, they offer us a doomsday benchmark,” he says. “They’re saying if we don’t get better at helping adults with autism and keeping them in their communities, if we don’t get better at delivering efficient, cost-effective care, then the economic toll is only going to increase.”
The researchers do consider a more optimistic scenario: If current spending on behavioral interventions for children with autism halves costs for young adults in 2025, then the cost of autism would drop by roughly $28 billion.
Optimizing these interventions for individuals could further lower costs. The new study budgets for expensive one-on-one interventions, which not all children need, says Connie Kasari, professor of human development and psychology at the University of California, Los Angeles.
“The cost of autism is huge, so we need to think about where we’re putting our energy. We need to improve those services in schools because those are the services for the majority of kids,” she says.
By joining the discussion, you agree to our privacy policy.