THIS ARTICLE IS MORE THAN FIVE YEARS OLD
This article is more than five years old. Autism research — and science in general — is constantly evolving, so older articles may contain information or theories that have been reevaluated since their original publication date.
Scientists have discovered a new way that microglia, the immune cells of the brain, can sculpt brain circuits, they reported today at the 2015 Society for Neuroscience annual meeting in Chicago. The cells release molecules that alter neuronal branching.
Microglia are molecular scavengers that engulf debris and pathogens, and are already known to prune connections between neurons.
“I think it’s important to keep in mind that microglia, in addition to being amazing scavengers, are also really good at producing signaling molecules,” says lead investigator Edward Ruthazer, associate professor of neurology and neurosurgery at McGill University in Montreal.
The researchers examined microglia in zebrafish larvae, which are transparent and allow scientists to follow brain circuits over time as they develop. They exposed the fish for two hours to a bacterial compound called lipopolysaccharide (LPS), which triggers an inflammatory response and activates microglia. Exposure to inflammation during brain development has been linked to autism.
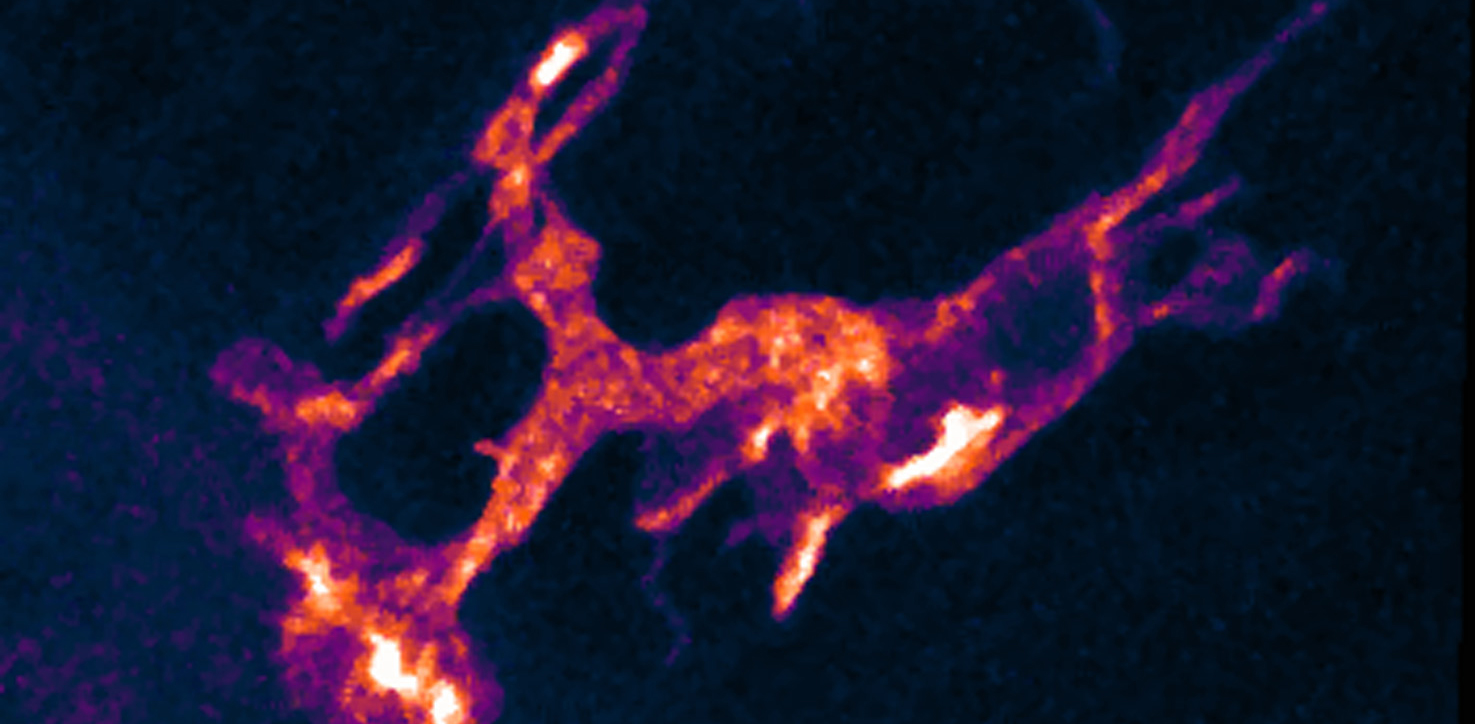
Exposure to LPS interferes with the formation of axons, neuronal projections that ferry electrical signals to other neurons, the researchers found. Over the course of four days following LPS exposure, axons that extend from the fish’s eye to the brain show an increase in the addition and removal of tree-like branches. They also have a greater proportion of transient structures, and a stunted rate of growth, compared with unexposed controls.
“Decreased overall growth with increased dynamics suggests to us a failure to stabilize synaptic contacts,” Ruthazer says. “It may represent failure of the axons to mature.”
Eyeing inflammation:
The researchers injected some fish with synthetic morpholinos — compounds designed to block the expression of specific genes — to prevent the development of microglia. These fish are protected from the LPS-triggered structural defects, suggesting that microglia play a key role in their formation.
However, brain imaging revealed that microglia are not in contact with the developing eye neurons, suggesting that the microglia play an indirect role in mediating the changes.
In addition to acting as garbage disposers, activated microglia are known to secrete inflammatory molecules. The researchers found that LPS exposure causes microglia to ramp up production of one such molecule, called interleukin 1-beta (IL-1beta). Deleting this molecule from the animals protects them from the LPS effects. Treating controls with it mimics the effects of LPS exposure.
“The microglia aren’t even necessary, once you deliver IL-1beta,” Ruthazer says. The results suggest that inflammation spurs microglia to produce signaling molecules that then act on the brain. The researchers do not yet know, however, how IL-1beta induces structural changes.
Still, the findings may provide insights into potential therapeutic targets. “If secreted inflammatory factors underlie aberrant circuit formation,” says Nasr Farooqi, a graduate student in Ruthazer’s lab who presented the findings, drugs targeting those factors might prevent or mitigate circuit problems.
For more reports from the 2015 Society for Neuroscience annual meeting, please click here.
By joining the discussion, you agree to our privacy policy.