THIS ARTICLE IS MORE THAN FIVE YEARS OLD
This article is more than five years old. Autism research — and science in general — is constantly evolving, so older articles may contain information or theories that have been reevaluated since their original publication date.
Having one child with autism raises the odds of having a second child with the disorder 20-fold, according to one of the largest epidemiological studies so far to address the inheritance of autism risk1.
The study, published 27 June in the American Journal of Psychiatry, found that this effect is greater for full siblings than it is for half-siblings, supporting genetics as a key factor in autism risk.
However, the study also hints at the importance of environmental factors. For example, the shorter the time between the birth of the child with autism and the birth of the sibling, the more likely the sibling is to have autism.
Half-siblings who share a mother also have a higher risk of having autism than those who share a father. This suggests that the uterine environment and other factors may contribute to autism risk.
“These kinds of results suggest to me that it’s probably a genetic-environmental interaction going on here,” says lead researcher Neil Risch, professor of biostatistics at the University of California, San Francisco.
The environmental component may be the most useful information for trying to reduce autism risk, Risch adds. “While the genetics provides important leads, it doesn’t provide immediate solutions.”
The new study is particularly valuable because it takes into account the fact that parents often refrain from having more children after having one with autism — a phenomenon called stoppage. A study published last year, which did not take stoppage into account, found only a sevenfold increase in autism risk for children who have a sibling with the disorder.
“The study benefits from the very large sample size and the ability to meaningfully contrast between different siblings and birth order without being hindered by stoppage,” says Elise Robinson, instructor in medicine at Harvard University, who was not involved in the study.
Sibling status:
The researchers looked at children who had received benefits through the California Department of Developmental Services. This approach is powerful because it involves all children with autism in a large geographical area rather than those at a certain clinic, says Aravinda Chakravarti, professor of molecular biology and genetics at Johns Hopkins University School of Medicine in Baltimore.
The researchers used birth certificates to link families and identify siblings. To account for stoppage, they looked only at siblings born after a child with autism. They began with 6,616 children with autism who have at least one full sibling, 644 who have a maternal half-sibling and 299 who have a paternal half-sibling. They directly compared these children with 29,384 typically developing children with at least one sibling.
About 10 percent of siblings of children with autism have the disorder, compared with 0.52 percent of siblings of controls, the study found. A 2011 study followed the outcome of infant siblings of children with autism and found that roughly 20 percent of the infants developed autism.
The new study’s estimate may be lower because it looked only at children who received services, and so may be skewed toward the more severely affected end of the autism spectrum, says Lonnie Zwaigenbaum, professor of pediatrics at the University of Alberta in Canada, who was not involved in the study. Severe symptoms are often the result of spontaneous mutations and are less likely to be inherited than are mutations with mild effects.
The study found that the risk is higher for the sibling born immediately following a child with autism than it is for those later in the birth order. The timing of birth is also important: “If the next child is born within a year or 18 months of the prior child [with autism], the risk is dramatically higher than if the couple waits, say, three or four years,” says Risch.
The reason for this trend is unclear, but it is consistent with evidence that exposure to byproducts of the immune system during gestation — which fade over time — may add to autism risk.
Two children born close together may also have other things in common, such as a pediatrician with a particular awareness of autism, so the explanation may be more straightforward than a complex environmental risk.
The fact that children who share a mother have about double the risk of those who share a father also points to environmental factors. (The study found only seven children with autism among the paternal half-siblings, but the difference is still significant.)
Still, genetic factors could explain this observation, researchers say. For example, females may need more genetic hits to develop autism than males do. That suggests that mothers who don’t have autism may carry some autism-linked mutations — the so-called female protective effect.
“The observations fit very well instead with protective effects in females,” says Kevin Mitchell, associate professor of genetics at Trinity College, Dublin, who was not involved with the study.
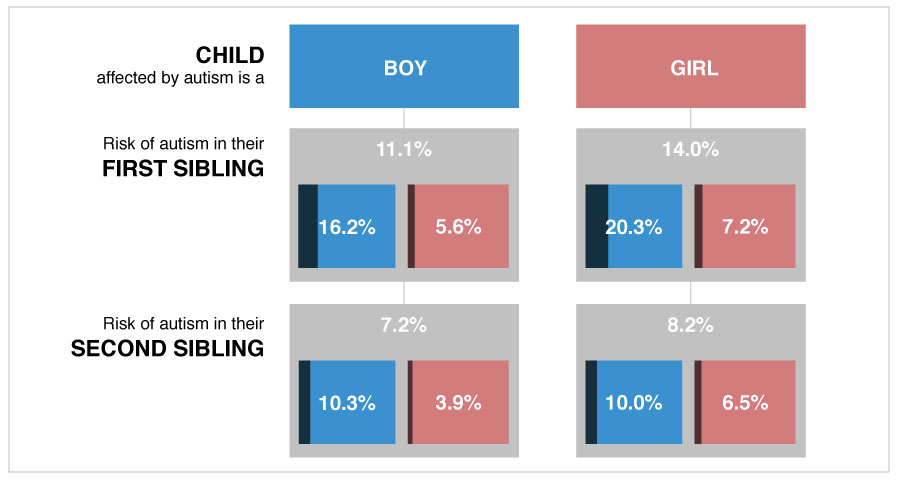
In fact, data from the new study may support this theory: The siblings of girls with autism (who presumably carry more mutations than do boys with autism) are 1.18 times more likely to have autism than the siblings of boys are — although this difference is not statistically significant. Risch says this effect is not large enough to account for the difference in risk between maternal and paternal half-siblings.
The debate is testament to the fact that autism risk lies in a foggy middle ground between genetics and environment.
“I have a hard time imagining a world in which one is true and the other is not,” says Robinson.
References:
1: Risch N. et al. Am. J. Psychiatry Epub ahead of print (2014) PubMed