THIS ARTICLE IS MORE THAN FIVE YEARS OLD
This article is more than five years old. Autism research — and science in general — is constantly evolving, so older articles may contain information or theories that have been reevaluated since their original publication date.
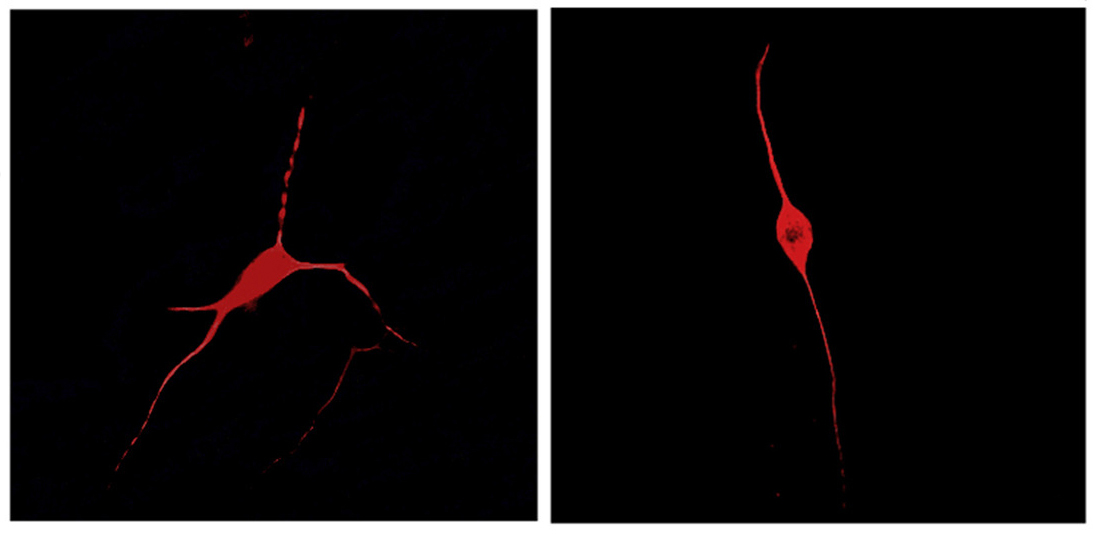
Star-shaped brain cells from children with autism release inflammatory molecules that harm neurons, a new study suggests1. Researchers derived the cells, called astrocytes, from the children’s teeth, and cultured them alongside neurons.
The new work hints that blocking inflammatory molecules from astrocytes could protect neurons in people with autism.
“There’s a chance that we could use this type of treatment in people,” says Patricia Braga, professor of genetics and embryology at the University of São Paulo in Brazil. Braga co-led the study with Alysson Muotri, associate professor of pediatrics and of cellular and molecular medicine at the University of California, San Diego.
Astrocytes support neurons and help to shape their connections, or synapses. But a string of studies over the past few years suggests that astrocyte function is altered in autism.
Braga and her team generated stem cells from dental pulp — the living tissue inside a tooth — from three children with autism and three controls. The children’s families had donated the baby teeth to the Brazilian Tooth Fairy Project, an effort to collect teeth as a source of stem cells.
A chemical cocktail coaxes stem cells to give rise to a mix of mature brain cells. After several weeks in culture, the cells form spheres of interconnected neurons and some astrocytes.
Neurons in the autism spheres have fewer branches than those from the control clumps, the researchers found. The autism neurons also form fewer synapses and show low expression of genes and proteins at the synapses. The results appeared 3 October in Biological Psychiatry.
The researchers probed the clumps of brain cells with tiny electrodes and found that autism neurons fire less frequently than control neurons do and release less glutamate, a chemical messenger that excites other neurons.
Mix and match:
The researchers also used another chemical cocktail to derive astrocytes. Again, they observed that autism neurons cultured with autism astrocytes assume a simpler shape than do control spheres. The autism neurons also signal poorly.
But in the presence of control astrocytes, the autism neurons grow branches and synapses, and regain normal signaling properties. Conversely, control neurons cultured with autism astrocytes form fewer synapses than usual.
“This study is a good proof of concept, showing that functional astrocytes can be generated and used to study the interaction between them and neurons in the context of brain disorders,” says Krishna Vadodaria, a postdoctoral fellow in Fred Gage’s lab at the Salk Institute for Biological Studies in La Jolla, California. “This can help tease apart the role of the astrocytes versus neurons in autism,” says Vadodaria, who was not involved in the study.
Braga’s team measured levels of the inflammatory molecule interleukin-6 (IL-6) in the cultures. Researchers have found elevated levels of IL-6 in blood, cerebrospinal fluid and postmortem brain tissue from people with autism.
Astrocytes derived from children with autism produce higher levels of IL-6 than those from controls, the researchers found. Blocking IL-6 improves the shape and function of the neurons.
The children with autism in the study all have repetitive behaviors, language impairment and sleep problems; none have seizures. The children do not have a mutation linked to autism and don’t share any genetic variants, however. This suggests inflammatory molecules produced by astrocytes play a role in multiple forms of autism.
“We focused on patients with exactly the same clinical phenotype, and found they have the same cellular phenotype, even though their genetic backgrounds are completely unrelated,” Braga says.
Braga and her team are exploring other inflammatory molecules released by the astrocytes. They are also testing the effects of anti-inflammatory drugs in cellular and animal models of autism.
By joining the discussion, you agree to our privacy policy.