
Illustration by Bobby Lopez
THIS ARTICLE IS MORE THAN FIVE YEARS OLD
This article is more than five years old. Autism research — and science in general — is constantly evolving, so older articles may contain information or theories that have been reevaluated since their original publication date.
Fragile X syndrome, tuberous sclerosis (TSC) and Williams syndrome are rare conditions with clear genetic causes: Each springs from a mutation in a single gene — and with unusual frequency seems to simultaneously produce a more common condition: autism1.
But is the ‘autism’ in a child with Williams syndrome the same as in a child with fragile X? And how does it compare with autism of unknown causes?
“This is a really difficult question because — is it the same thing as what? We don’t have a model autism case,” says Bonita Klein-Tasman, professor of psychology at the University of Wisconsin-Milwaukee. “We have a pretty broad umbrella of what we consider to be autism right now.”
In terms of genetics, autism research is much more sophisticated than it was just a few years ago. Scientists have identified a few dozen genes that seem to be important players, and are hot on the trail of these genes’ malfeasance. But along with this increasing clarity, an existential crisis is emerging: What, exactly, is autism?
“Certain folks think that autism is a thing,” says Raphael Bernier, associate professor of psychiatry at the University of Washington in Seattle. “I don’t think so. We’re defining it a certain way and there are a lot of different ways to get there.”
Social subtlety:
Some element of this uncertainty has always accompanied autism. Note the common saying: “If you’ve met one child with autism, you’ve met one child with autism” — a testament to the condition’s maddening diversity.
Some children with autism are social but awkward; others are socially withdrawn. Some don’t speak at all; others are hyperverbal. Some tune out all distractions and can focus intensely; others seem hyperactive and easily distracted.
The advances in genetics over the past few years have only confirmed this variability. As researchers identify people with autism who share the same rare genetic mutation, they are finding that each subgroup has its own distinct profile, with differences even among members of the same subgroup.
“If we had good clinical data on 50 patients for each of the 500 or more predicted single-gene causes of autism, they’d probably all have a different profile,” says David Ledbetter, chief scientific officer at Geisinger Health System in Danville, Pennsylvania. “They’ll each have their own social communication and cognitive profile.”
Bernier brings children to his clinic from all over the world who bear rare mutations in any of a set of genes strongly linked to autism. Grouping these children by the mutation they carry, he paints portraits of their common features. For example, children with a mutation in CHD8 tend to have wide-set eyes, large heads and trouble socializing. Many of them have what Bernier describes as “waiting-room autism” — meaning their autism can quickly be identified by sight alone: “I’m seeing a kid who is not engaged with others, who is not using broad facial expressions, not making eye contact.”
By contrast, children who carry a deletion in the 16p11.2 chromosomal region seem interested in socializing, but awkward, Bernier says. “Many of them have social quirks and oddities, but they’re not that waiting-room autism,” he says. “They are socially motivated and engaged but don’t know what to do once they are engaging with someone.”
Unknown origins:
Estimates of the genetic contribution to autism vary widely. One study, published this year, indicates that as much as half of all cases of autism derive from harmful, spontaneous mutations in single genes2. Other estimates suggest a more significant role for combinations of milder mutations present in the general population3. No single autism-linked mutation seems to contribute to more than about 1 percent of autism cases, however.
For years, many researchers considered idiopathic autism — meaning autism arising from unknown causes — to be separate from the condition seen in genetic syndromes such as fragile X or Williams (see graph). That perception is changing.
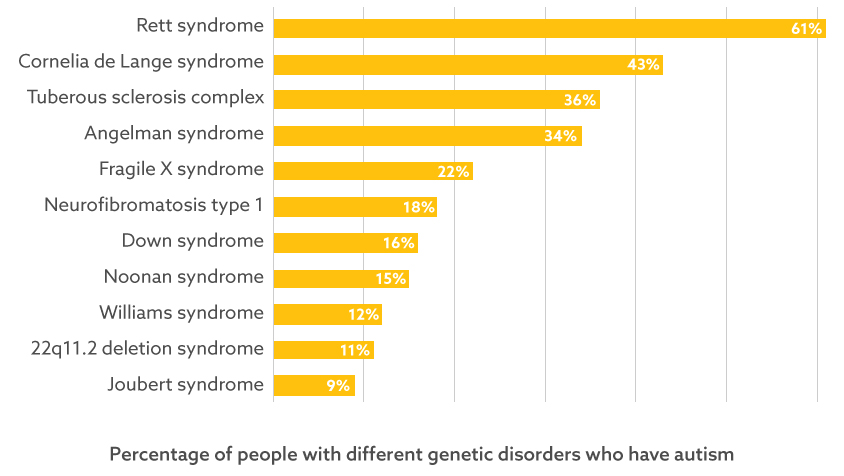
Contiguous conditions: A meta-analysis of 158 different studies generated prevalence rates of autism across 16 genetic syndromes (11 shown here). The analysis weighted studies based on the number of participants and rigor of diagnostic methods used.
Nigel Hawtin
“In the past, people used to segregate syndromic autism from idiopathic, or ‘pure,’ autism. It’s pretty clear that this distinction is getting blurred now,” says Mustafa Sahin, associate professor of neurology at Children’s Hospital Boston. “At the neurological and circuit level, it seems that they are converging.”
One reason why disorders such as fragile X syndrome seem only peripherally related to autism is that not everyone with a mutation in the fragile X gene has autism. But as researchers identify more autism mutations, it is becoming clear that this variability in symptoms may be the rule rather than the exception.
For example, only about 25 percent of people with a deletion in the 16p11.2 chromosomal region have autism. But a closer look reveals that all of them have social deficits when compared with their parents, says Ledbetter4.
Klein-Tasman works with children who have both autism and Williams syndrome, a disorder characterized by excessive sociability and intellectual disability. Some of these children display autism traits — social communication challenges and repetitive behaviors — well in excess of most children with Williams syndrome, says Klein-Tasman. This is often the case with other syndromes as well: The children who meet the bar for an autism diagnosis have more severe social deficits or repetitive behaviors than those who have only the related syndrome.
In these cases, Klein-Tasman says, more than one gene may be at play. “My hypothesis would be that these [more severely affected] kids have a double hit,” Klein-Tasman says. “They have Williams syndrome and probably some other vulnerability for an autism spectrum disorder.”
Clinicians often stop looking for mutations once a child has tested positive for a known genetic syndrome. But a few researchers are taking a second look at these cases. For example, Thomas Bourgeron at the Institut Pasteur in Paris is sequencing the entire genomes of people known to have one strong autism mutation, with the goal of uncovering additional mutations.
Predictive patterns:
Adding to the complexity in studying autism’s shape is the fact that its symptoms may change as children grow up.
In a 2009 study, Klein-Tasman and her colleagues found that more than half of 30 children with Williams syndrome have autism diagnoses at ages 2 to 55. But an unpublished study from the same team shows that once children can speak in phrases, the proportion of autism diagnoses drops to around 25 percent. This may be because as children begin talking, their interest in socializing becomes more apparent.
To get a better picture of autism, researchers should focus on how it evolves over time, Klein-Tasman says. “We tend to get these snapshots of a single point in development. Maybe what we’re going to find is there’s a prototypical autism in the developmental trajectory.”
Following children during development may also help reveal how autism emerges in the brain. Sahin is exploring this question in children with TSC, a condition marked by benign tumors throughout the brain and body.
Roughly 50 percent of children with TSC develop a characteristic form of autism, says Sahin. Studies suggest that brain patterns in children who have both TSC and autism are more typical of children with autism alone than they are of children with TSC alone6.
Sahin and his colleagues are scanning the brains of 120 children with TSC from infancy to 3 years of age, when they can be reliably assessed for autism. It may be that disparate ways of arriving at autism lead to a similar set of changes in the brain, Sahin says.
This study, along with many others, aims to uncover a biological indicator of autism. The researchers hope to pin the condition down with more than just the behavioral assessments currently used.
“We’re defining autism as impairments in social communication interactions or repetitive behaviors that someone deems to be problematic,” says Bernier. “It’s so tricky, because when you define things behaviorally like that, it makes it difficult to say what something really is.”
By joining the discussion, you agree to our privacy policy.