Spectrum: Autism Research News
The measure of a life
Terms such as ‘low-functioning,’ often used to describe people with autism, are misleading and stigmatizing. Tracking people’s daily lives over time may offer a clearer picture of life with the condition.

Alex Garish knows how to make a dramatic entrance. The 11-year-old glides into the dining room of her family’s home in northwestern Montreal, arms outstretched like a plane, making a soft whooshing sound. She dips and turns abruptly before coming in for a smooth landing on the wicker chair in front of the family computer. With a few flicks of her fingers, she launches an animated video about circles, squares and other geometric shapes, and is immediately engrossed. Now and then, she turns to glance furtively over her shoulder at a visitor seated at a table behind her.
Alex was diagnosed with autism at age 2 and didn’t talk until she was over 4. Today, she speaks only in simple two- to three-word sentences. Standardized tests reveal that she is mildly cognitively impaired. She has trouble bathing and using the toilet by herself. She cannot tell time, and needs help crossing the street. When she is upset, she throws violent tantrums, often hurling objects across the room or flinging herself onto the floor.
On the other side of the St. Lawrence river in Montreal lives John Walsh, a 13-year-old boy who was diagnosed with autism at age 3 and, like Alex, was slow to develop speech. (John’s mother, Mary Walsh, asked that we not use their real names, as John does not acknowledge that he has autism.) But unlike Alex, John shows no signs of cognitive impairment. At his school, a mainstream one for typically developing children, he excels at reading and math. He uses public transportation on his own and can even give strangers directions on the city’s complex subway system. John easily carries on conversations, though he tends to take things literally, and certain phrases, such as ‘catch the bus,’ trip him up.
Alex’s parents describe her as ‘low-functioning,’ whereas John’s describe him as ‘high-functioning.’ But these labels can be misleading.
“Parents often ask around the time of diagnosis, ‘Where on the spectrum is my child; is he at the high or low end?’” says Tony Charman, professor of clinical child psychology at King’s College London. “You sort of do know what they’re asking, but you don’t [really know]. Are they asking about ‘autism severity’? Are they asking about functioning or everyday adaptation?”
Despite her difficulties with language and cognition, for example, Alex does just fine with many parts of everyday life. Most weekdays, she goes to a school for children with autism or other special needs. As soon as she gets home each day, she darts up the stairs to her room and quickly changes into play clothes without any help. She keeps her room neat and organized. Dozens of her original drawings cover the walls of her bedroom. She rattles off the full names of her favorite composers: Wolfgang Amadeus Mozart, Johann Sebastian Bach and Ludwig van Beethoven. When she senses that her younger brother is hurt, she rushes to his side, carrying a makeshift doctor’s kit to try to fix whatever ails him.
Alex often leads the other children in her class in their dance routines, and her mother, Wendy Garish, boasts that a teacher calls Alex one of the best dancers in the class. Alex has even forged friendships with a few others in her class, and has lunch every Wednesday with a boy she particularly likes. “They love each other,” Wendy says. “When they walk together, she grabs his hand.”
By contrast, although John does well in school and excels at many aspects of daily life, he seems to struggle in ways that are not immediately obvious. He has no friends and has trouble interpreting other people’s facial expressions and recognizing emotions from the tone of a person’s voice. During gym class, he walks the lines of the gymnasium floor rather than playing games with others. He can be inflexible, one of the hallmarks of autism. For example, he wears only a certain colored shirt on each day of the week: blue on Mondays and orange on Fridays. But his school requires students to wear only black and white, a policy that at first caused him tremendous anxiety. Until he got used to the rule, John would cope by wearing his colored shirt underneath his black-and-white uniform, which he peeled off as soon as he got home.
It’s clear that Alex and John each function well in certain areas of life and struggle in others; each has an idiosyncratic patchwork of skills and challenges. Their stories illustrate a problem that has plagued autism research for decades: What, exactly, do the terms high- and low-functioning mean and to whom do they apply?
An ongoing study in Canada may be able to help answer this question. Since 2004, a team of researchers at five universities has been tracking more than 400 children with autism, including Alex and John, since they received their autism diagnoses. They are characterizing the children by their developmental trajectories — how their symptoms and abilities in multiple domains change over years and even decades. The long-term study may help explain why these two children diverged in their skills despite starting out with similar ones at the time of diagnosis. It may also explain how the traditional labels need to evolve to accurately describe children with autism.
Other teams are developing multidimensional techniques for measuring how well a person with autism functions in different aspects of daily life — from communicating with others to the ability to participate in a community. These new tools may provide a common language, so that researchers, clinicians and families can more easily understand one another. They may point the way toward personalized treatment by pinpointing individual deficits. But beyond those practical goals, they may also provide a dramatically richer, more holistic sense of what it is like to be a person with autism.
“The term ‘low-functioning’ is just awful.” Catherine Lord
Limited by labels:
In studies of autism, the term ‘high-functioning’ is often used to describe a person with autism who scores above 70 or 80 on intelligence quotient (IQ) tests. Scientists sometimes exclude those who score below this cutoff from their autism research because the participants may have difficulty following instructions or completing the study.
But relying on IQ is a crude approach, says Peter Szatmari, chief of the Child and Youth Mental Health Collaborative at the Centre for Addiction and Mental Health and the Hospital for Sick Children in Toronto, who leads the long-term Canadian study. “It’s not a measure of functioning; it’s a measure of whether or not they’ve got intellectual disability,” he says. “It doesn’t reflect how kids with autism do in the real world.”
Some researchers instead use symptom severity as a metric: For example, they might label as low-functioning a child who frequently avoids interacting with others and flaps his hands a lot or shows other repetitive behaviors and restricted interests.
Meanwhile, parents of children with autism often judge functioning using criteria such as how well their child talks, or how easily he or she participates in activities. Parents sometimes resort to using terms such as low-functioning as a shorthand to indicate a child who has some impairments, without having to spell out exactly what those impairments might be, says Catherine Lord, director of the Center for Autism and the Developing Brain at New York-Presbyterian Hospital. “Sometimes in the press, the focus is so much on the people with autism who can speak for themselves, and who do very exciting things, so the families want to be clear this is not the child that they have.”
But the label can trap children in a category that is often stigmatizing. “The term ‘low-functioning’ is just awful,” Lord says. “It doesn’t mean that they can’t do things — it just means they need more support.” (In the U.S., the diagnostic manual rates autism severity by the level of support an individual needs, rather than by her abilities.)

Clear interests: Alex Garish enjoys blowing bubbles in her family’s living room when she gets home from school.
Photos by Marie-France Coallier
Even being tagged as high-functioning can have unfortunate consequences. Any person, regardless of whether they have autism, functions better in some areas of life than in others, whether that’s making and keeping friends, learning and remembering information, taking care of themselves, communicating, solving problems or paying attention. Saying a person with autism is high-functioning implies they are competent in all of these areas, but that’s simply not true, Charman says. “Someone could be very bright on an IQ test but be very socially impaired and have enormous problems in forming relationships or managing within the environment because of sensory sensitivities or high levels of anxiety.”
In practical terms, either label can be limiting: It might prevent one child from participating in activities she wants to do, or exclude another from getting the services he needs.
But simply abandoning labels altogether isn’t an alternative. Researchers need some sort of language to describe the different manifestations of autism, says Lord. “The trouble is, as human beings, we like abbreviated terms,” Lord says. “But it would be nice to have something other than ‘high-functioning’ and ‘low-functioning.’”
Multiple paths:
Szatmari’s study may provide some alternatives. The idea for the study germinated in the 1990s, long before Alex and John were even born. Szatmari and his colleagues wanted to design and conduct a study that would address the research priority of the broader autism community, which includes parents, clinicians and policymakers. They surveyed the community to assess priorities, and the most popular suggestion came as a surprise.
“I thought it would be a study on what’s the most effective form of early intervention, or what’s the best treatment,” Szatmari says. Instead, the question that came up most frequently was: ‘What factors are associated with a good outcome?’ In other words, what determines how well a person with autism will function in life?
To answer the question, Szatmari and his team launched the Pathways in Autism Spectrum Disorders study to track children diagnosed with autism between the ages of 2 and 4. Because few researchers agree on what a good outcome looks like in people with autism, the team decided at the outset not to focus on any single domain, instead tracking the children in a variety of areas.
“There are many different kinds of so-called ‘good outcomes,’” says Mayada Elsabbagh, assistant professor of psychiatry at McGill University in Montreal, who works with Szatmari on the study. “Our challenge is how to capture as many as possible in domains we already understand and believe are relevant.”
Four times during the first four years and roughly every two years thereafter, the researchers have measured the children’s cognitive abilities, language skills and severity of autism symptoms with standardized tests. Parents and caregivers complete questionnaires that ask about their own stress levels and coping methods and their child’s daily living skills, behaviors, symptoms and treatments.
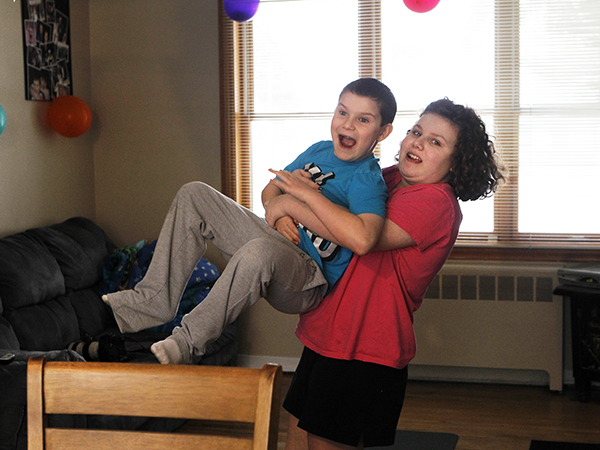
Fast friends: Alex often roughhouses with her younger brother, Max, and has even made a few friends at her school.
One goal of the study is simply to describe how the children’s symptoms, skills and abilities change as they grow up, and to determine whether they fall into subgroups based on these trajectories. Another aim is to figure out whether certain characteristics at baseline — such as IQ score, language ability, gender or age at diagnosis — can predict how a child will change over time.
Already, the initial phase of the study has brought new insights about how symptom severity and daily living skills may change in the children from the time of diagnosis up to age 6. (The second phase, for which the researchers finished collecting data last year, looks at how the children functioned up until 11 to 12 years of age; a third phase aims to follow the children until they are 18.) After analyzing four years’ worth of data, Szatmari and his colleagues reported last year that they could divide the children into two groups based on the severity of their symptoms, including social and communicative impairments, repetitive behaviors and restricted interests. Most of the children had severe symptoms at the time of diagnosis and changed little as they grew up. A smaller group, 11 percent, began with relatively mild autism symptoms that improved over time.
Next, the team looked at skills of daily living, also known as adaptive functioning — how well the children communicate and interact, whether they can make a phone call or use the Internet, their ability to eat, dress, bathe and brush their teeth, and how well they understand concepts such as time and money. One group, including 29 percent of the children, had the poorest daily living skills, which worsened with time. A second group — half of the children — had moderate functioning levels that remained stable. The third and smallest group of the children had the strongest abilities at diagnosis and improved with age.
Surprisingly, the researchers found little overlap between the two sets of groups. The children with the most severe symptoms did not necessarily belong to the group with the poorest daily living skills, suggesting that symptom severity has little to do with performing everyday tasks.
This finding reflects what parents often report: Some children with autism, like Alex, might have narrow interests and struggle to talk, but they still manage to take care of daily tasks. It also reaffirms that one single measure of functioning cannot predict how well a child performs in other areas.
Some clinicians look to the severity of autism symptoms to determine which children with autism need treatment the most, and might use it to gauge whether a treatment is effective. Szatmari says his study calls these practices into question. “We should be focusing on how they are functioning and doing in the real world and if their symptoms get in the way of that, okay, but if they don’t get in the way of that, then don’t worry about it.”
Not everyone is convinced that symptom severity and daily living skills are totally independent of each other, however. Lord says Szatmari and his colleagues controlled for differences in language ability and age when they measured symptom severity, but only controlled for age when assessing daily living skills. That means they cannot directly compare the two types of scores, she says. (Szatmari says the children started out with similar language abilities at the start of the study, but he did not comment on how language differences later in life could affect the findings.)
In any case, by demonstrating the inherently dynamic nature of autism, Szatmari’s findings point to the weakness in using the same label to describe a child throughout her life. Most studies that brand children with autism as high- or low-functioning do so based on IQ as measured at a single point in time. But “kids can change with respect to their baseline, and they can also even change in terms of how they compare to other kids,” says Lonnie Zwaigenbaum, co-director of the Autism Research Centre at the University of Alberta, who works with Szatmari on the study. Because of this, it may be inappropriate to judge the functioning level of a child with autism based on a single measure early in childhood.
With data from only the first phase of the study analyzed, it’s too soon to say which factors in early childhood predict how a child will fare over time. So far, the researchers have reported that the boys in the group tend to have stable autism symptoms throughout childhood, whereas the girls tend to start out with mild symptoms and improve with age. What’s more, the children who were diagnosed early or who had a high baseline IQ or good early language skills seem to also have good daily living skills that improve over time.
In Alex’s case, for example, her communication and social skills have improved dramatically over the past three years, says Wendy, her mother. Alex’s parents are growing more confident in her ability to fend for herself around the home, too. Alex still needs help bathing and using the bathroom, but she has few difficulties picking out and putting on her clothes, brushing her teeth, putting herself to bed and feeding herself prepared foods.
One night in February, for example, Wendy put a plate of chocolate chip cookies on the table, and Alex immediately bounded over to investigate. She held a cookie to her nose and inhaled deeply. A look of disgust flashed across her round face, and she dropped the cookie back onto the plate, spun around and strode out of the room. She began rummaging around in the freezer, then returned to the dining room carefully tearing off the wrapper of an ice cream sandwich. It seemed pretty clear that she knew it was time for family dessert and had figured out a way to participate even though she didn’t want what everyone else was having.
Still, Alex’s parents worry that her ‘low-functioning’ label might be hindering her development. Alex enjoys swimming, for example, but her parents say they have seen advertisements for swim lessons that can accommodate only high-functioning children with autism.
“She can swim — she might swim even better than your high-functioning kids,” says her father, Peter Garish. “It’s only because they’re worried that low-functioning means more attention has to be given to them. They’re automatically equating low-functioning with not being able to do the same things.”
“When we introduce this idea of strengths, it’s refreshing to [parents].” Briano Di Rezze
New measures:
Last summer, Szatmari’s team secured funding to continue following the children until the age of 18. As the researchers gear up to assess children who are moving into adolescence, they are thinking about environmental influences that may shape how a person with autism fares in life. They are exploring how factors such as entering high school, socioeconomic status, ethnicity, use of support services, and parental mental health influence functioning over time. “A lot of studies in autism are very focused on the individual kid with autism and their symptoms, IQ and language — variables that are inside the kid,” Szatmari says. “We have a more holistic view.”
So far, the researchers have focused on abilities they can quantify: symptom severity, IQ, skills and behaviors. Elsabbagh has plans to explore more intangible measures.
ASD Voices, a subproject of Pathways, aims to collect the children’s first-person perspectives on their hopes and dreams, interests, feelings and thoughts. The details are being worked out, but the team plans to interview those children who can communicate in words and, for those who cannot, offer alternative modes of expression such as drawing and photography. The researchers’ goal is to learn what each child considers to be a ‘good outcome’ and compare that with the types of outcomes studies traditionally measure. The people best able to describe what a good outcome looks like would be the kids themselves, Elsabbagh says.
Other teams are also exploring methods to probe functioning beyond binary high/low measurements. For example, researchers at the Karolinska Institute in Sweden are developing a standardized test to capture a comprehensive profile of functioning in children with autism.
The team’s work draws on the International Classification of Functioning, Disability and Health (ICF), a massive tool developed by the World Health Organization to assess how any health condition affects daily functioning. The ICF measures people on a scale from 0 to 9 for more than 1,400 items spanning how severely a health condition affects their body and their ability to fulfill everyday activities, as well as how environmental factors — such as relationships and access to support services — improve or worsen their daily life.
Because the ICF is so exhaustive, it is impractical for scientists to use it regularly. To make it more useful, the Karolinska team, led by neuropsychiatrist Sven Bölte, is whittling down the items to form so-called ICF Core Sets for Autism Spectrum Disorder, looking specifically at brain function, communication, social skills and relationships. Bölte says anyone will be able to use these core sets to create an inventory of the strengths and limitations of a person with autism, rather than combine measures from a mishmash of diverse tests.

Uncertain future: Alex’s mother, Wendy, remains optimistic that Alex will one day hold a job.
Another team, at McMaster University in Hamilton, Canada, is devising a method for classifying children with autism based on how well they communicate in everyday life. This approach builds on a tool for classifying motor function in children with cerebral palsy developed 20 years ago.
The method focuses on social communication because interviews with a group of autism experts indicated that this domain of functioning is the most important in developing a classification system, but researchers could develop similar schemes for other areas of functioning, says Briano Di Rezze, assistant professor of rehabilitation science at McMaster University, who leads the project. The classification system uses five short paragraphs to describe levels of ability. For example, level 5, the lowest, describes a child who rarely interacts with others and talks only to himself, indicating that he doesn’t grasp the point of communication, whereas a child at level 1 can participate in conversations and relate to others.
Di Rezze says the system should be quick and easy for anyone to use, giving researchers, teachers and parents of children with autism a common language to talk about how a child is functioning. If a teacher rates a child differently than the child’s parents do, that might open the door to talking about the differences between home and school. “Maybe there’s something that’s happening in school that we can address to help,” Di Rezze says.
Each of the new tools might allow doctors to pinpoint a child’s specific support needs. Each also focuses on what people with autism can do rather than on what they cannot, notes Zwaigenbaum. “I do think that’s still a major advance from how we’ve historically defined functioning in autism,” he says.
This shift in focus may also reduce the stigma of autism and help doctors build rapport with families. “The medical and health system is set up to address medical issues, and so it’s hard for parents to talk about what their kids are good at because they’re so focused on deficits,” Di Rezze says. “When we introduce this idea of strengths, it’s refreshing to them.”
Indeed, the parents say this new emphasis on abilities is welcome.
John’s mother, Mary, is encouraged by how much her son has changed since his diagnosis. John may go to college, and maybe one day even become a lawyer. But above all else, she says, she wants him to be happy and feel connected to society.
She sees his restricted interests less as a limitation that needs to be fixed and more as a quirky asset, to the point that his lack of friends no longer concerns her. “That does not bother him, so why should it bother me?” she says. “Just because my son is into clocks, metros, politics and different kinds of aircraft doesn’t mean he needs to be cured of that; isn’t it neat that some people have these bizarre focuses?”
Alex’s parents also say that focusing on her strengths, and her progress during the past few years, helps them to remain optimistic even though they have no idea exactly what the future holds for her.
They fear Alex will be taken advantage of and that it is unlikely she will ever live on her own. Still, she has made so much progress over the past three years, Wendy says, that she hopes Alex will one day hold a simple job — perhaps one that makes use of her computing skills — that gives her some sense of accomplishment. “I’d be very happy with that, just so she’s part of society.”
By joining the discussion, you agree to our privacy policy.